
Developing a Patient Navigation Program to Improve Treatment Outcomes for Patients with Breast Cancer at Butaro Cancer Center of Excellence (BCCoE) in Rwanda
Breast cancer is the most prevalent cancer among women worldwide, with approximately 2.3 million new cases and 764,000 deaths annually (Bhangdia et al., 2026). While high-income countries (HICs) have high incidence and relatively low mortality, low- and middle-income countries (LMICs) have lower incidence but disproportionately higher mortality (Force et al., 2025). This disparity is largely driven by limited cancer care infrastructure and inadequate access to timely screening, diagnosis, and treatment in LMICs (Akinyemiju et al., 2022). Even when early diagnosis and treatment initiation occur, treatment noncompletion remains a substantial issue, leading to preventable deaths.
Patient navigation programs (PNPs) are an evidence-based strategy to improve diagnostic timeliness and treatment adherence in cancer care. These programs guide patients through complex health systems, address barriers to care, and provide personalized support across the care continuum (Chen et al., 2024). Although PNPs were developed primarily in high-income settings, the World Health Organization (WHO) recommends them as a key strategy to improve breast cancer outcomes globally (WHO, 2024). However, evidence to guide their adaptation to the specific contexts and needs of LMICs remains limited.
Sub-Saharan Africa exemplifies these challenges. Prospective cohort studies have documented high rates of treatment abandonment across multiple African countries (Foerster et al., 2022) and significant non-completion of surgery and chemotherapy in Rwanda (Bhangdia et al., 2025). Research indicates that providing women worldwide with access to quality cancer care could prevent 34% of annual female cancer deaths (Ginsburg et al., 2023), underscoring the urgent need for effective interventions in resource-limited settings.
To inform the adaptation of PNPs for LMICs, we conducted a formative study to design and tailor a patient navigation program for the Butaro Cancer Center of Excellence (BCCoE) in Rwanda, building on existing navigation-related services. The study demonstrates that a context-sensitive, patient-centered PNP can be developed for resource-limited settings and offers an approach applicable to similar contexts in LMICs.
Learn more about this thesis project: Join us for the Class of 2026 MMSc-GHD Thesis Presentations May 11–13. Register for the Zoom. See the schedule of presentations.
Photos and reflections on the thesis project
Students submitted photos and reflections as part of their thesis research. All the people in the photos gave permission for their photos to be taken and shared.

Directional sign at Butaro Cancer Center of Excellence (study site) indicating the infusion center, where breast cancer patients meet their clinical team for consultations and receive chemotherapy. Another sign directs patients to a support center that offers short accommodations for those staying overnight, either waiting for their next-day chemotherapy or receiving treatment on the same day, but are unable to travel long distances home afterward. These signs exemplify the biosocial approach essential for holistic breast cancer treatment in rural areas with limited accommodation and transport options. Photo Credit: Aimable Uwimana

Study Data Collection Team—Chantal Uwimana (left), Gasaro Sharon (left), both data collectors, and Vivens Nsabimana (right), research assistant—pause on the Butaro Level Two Teaching Hospital (BL2TH) sign during their lunch break amid data collection. The Butaro Cancer Center of Excellence (study site) is located within BL2TH. Photo Photo Credit: Aimable Uwimana

A 57-year-old breast cancer patient referred from the Western Province of Rwanda arrives at the Butaro Cancer Center of Excellence in Northern Rwanda seeking cancer care after an eight-hour journey on multiple connecting public buses. This photo highlights the geographical and logistical access barriers many women with breast cancer in rural Rwanda face, some of which have the potential to be addressed by patient navigation services.

A Focus Group Discussion (FGD) is underway with the Butaro Cancer Center Oncology Staff to examine barriers and facilitators to implementing a Breast Cancer Patient Navigation Model at the Butaro Cancer Center of Excellence. A trained study research assistant facilitates the FGD, while Kamanzi (the student study PI) follows online. This photo highlights opportunities for qualitative data collection methods when geopolitical travel restrictions limit the student PI’s ability to travel to the study site for in-person data collection.
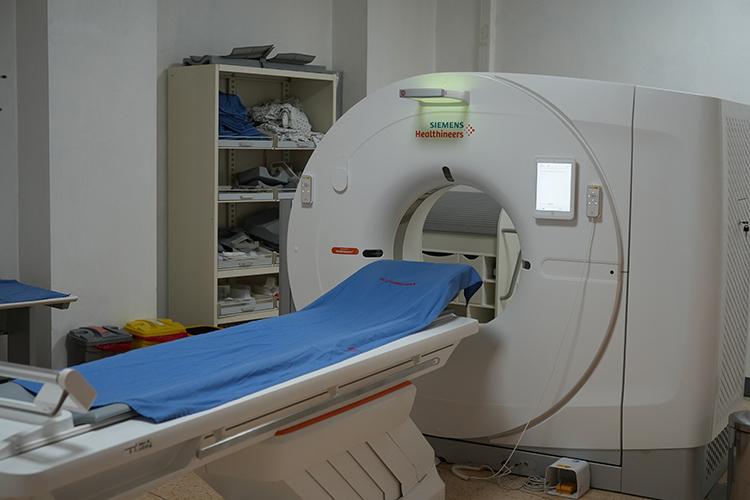
In July 2024, the Butaro Cancer Center of Excellence (BCCoE) installed its first CT scan machine. CT scans are vital for diagnosing and staging breast cancer. Before getting the machine, patients had to travel over 60 miles to Kigali, the capital, for scans, which was time-consuming, costly, and caused delays in treatment. Since the CT scan became available, there has been a notable decrease in referrals for breast cancer diagnosis.

